
By Kris Herndon
In April, Dr. Scott Wolfe, a hand surgeon, performed the first wrist-replacement surgery using a new implant he designed.
Dr. Wolfe, a Greenwich resident, is chief emeritus of Hand and Upper Extremity Service at the Hospital for Special Surgery (HSS) in New York.
The new implant, called the KinematX™ Total Wrist Arthroplasty System, has just been cleared by the FDA.
Wrist replacement surgery isn’t new. But implants for other major joints, such as knee and hip, are more common – and have historically been much more successful. For wrist replacements, though, “the failure rate was over 50%,” Dr. Wolfe says.
As a specialist whose patients have included world-class musicians and athletes, restoring total mobility to the hand and wrist is a top priority for Dr. Wolfe. But older wrist implants tended to wear out or cause pain, leading to repeated surgeries to correct the problems.
“We needed to build a better mousetrap,” says Dr. Wolfe.
To fully understand why existing wrist implant designs weren’t succeeding, Dr. Wolfe and his co-inventor, Dr. Joseph J. (Trey) Crisco, spent decades studying the movement of the human wrist.

“There is a particular motion called dart-throwers motion,” Dr. Wolfe explains. “Our research showed that it’s a unique motion of the human wrist. Apes don’t have it. And it may well be much more important than the opposable thumb, in terms of what separated us from the other hominids out there.”
Once prehistoric man evolved that motion, Dr Wolfe explains, he gained multiple survival advantages. He could throw rocks or swing a club to defend his young, and he could use tools in a more complex way. What’s more, he could throw a spear to hunt meat.
Hunting meat was a game-changer, says Dr. Wolfe: “In doing so, we became carnivores, which in turn allowed brain size to increase. And the rest is history.”
As it turns out, the dart-throwing motion is also one reason older wrist implants fail. They aren’t designed for that kind of complex, fluid motion — which occurs as part of a multitude of normal human activities, from golfing and fishing to beating eggs, pouring a cup of coffee, or driving.
“If patients are trying to do those activities, and their prosthesis won’t let them – if it impinges that motion, or is resisting that motion — it’s going to transfer all those energies to the interface,” Dr. Wolfe explains.
That means wear and tear where the implant meets the bone – which, in turn, leads back to that 50% failure rate for wrist implants.
One reason the human wrist is capable of such complex motion is that it is actually comprised of two joints. Having analyzed dart-thrower’s motion, Dr. Wolfe and his co-inventor, Dr. Crisco, had an epiphany when they began considering those two joints separately. They realized that what’s called the midcarpal joint, where the radius bone joins the first of two rows of wrist bones, is the locus of such complex movements. That was the joint they needed to duplicate in order for the new implant to succeed.
“It was a big a-ha moment,” Dr. Wolfe recalls. “And so, the design of the prosthesis basically emulates that particular joint, and, in so doing, it allows the dart-throwing motion.”
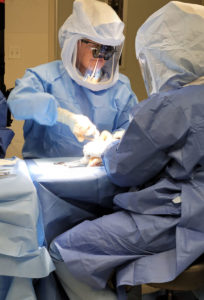
Mark Eisen, a Georgia resident who traveled to HSS for the surgery, is the recipient of the new KinematX™ Total Wrist implant. Eisen suffered from severe arthritis in his right wrist, and, when he sought treatment way back in 2011, he wasn’t satisfied with the options described by his regular physician.
“Basically, either they take the wrist bones out, or they fuse them together,” Eisen recalls.
One common result of either type of surgery is limited mobility, or, as Eisen sums it up: “If it hurts when you move it, don’t move it.”
“I didn’t really like that solution,” said Eisen, who is an avid golfer and hoped to resume his ordinary activities to some extent. Frustrated, he turned to the Internet. “I’m really good at Google,” he says, laughing. “I started doing some research.”
His research led him to Dr. Wolfe, who at that time, in 2011, had performed several midcarpal hemiarthroplasty surgeries, using an implant – the first-generation design that would later give rise to the new KinematX™ Total Wrist implant design — that replaced half the wrist joint.
Dr. Wolfe and Eisen began corresponding about Eisen’s case. Eisen recalls: “Pretty early on, I realized, you know, this guy is one of the top guys in the world for this. He told me about the KinematX™ implant and where it was going, and I said, ‘Look, I’ll wait.’ But I didn’t think it was going to take seven years!”
But with Eisen’s other options so unsatisfactory, he kept monitoring Dr. Wolfe’s work. “Over the seven years, I would email Dr. Wolfe and he’d always email right back.”
Indeed, Dr. Wolfe had taken an interest in the case: “Mark’s case was different from the average in that it had been going on since he was a young kid. And in the process, his wrist had collapsed quite a bit. Some of the bones were eroded; all of them were rotated out of position.”
Eisen’s bones had degenerated, and cysts were present. “Those are fluid-filled spaces in the bone, and they don’t support the prosthesis very well, so we have to remove them,” Dr. Wolfe explains. “When you’re doing a total prosthesis, you have to cut off the portions of the bone that have degenerated, leaving behind the portions that are still very healthy. It sounds easier than it is,” Dr. Wolfe says with a rueful laugh. “Those cuts have to be very precise.”
Dr. Wolfe knew he needed twelve millimeters of healthy bone, and after removing the cysts, they were down to about thirteen. “So we were really cutting it close. We had to have a back-up plan, which was to use cement.”

Polymethyl methacrylate (PMMA) bone cement is common in fixing implants to bone; indeed, until fairly recently, it was the only option. “But it’s not ideal. It generates heat; it can actually burn the bone. And it’s inert,” Dr. Wolfe says. “The bone doesn’t grow into it.”
The preferred option for the KinematX™ interface, if enough of Eisen’s remaining healthy bone could be preserved, was to apply a porous coating only a millimeter or two thick. “It’s shaped a lot like normal bone, so the bone recognizes it, and grows through it,” Dr. Wolfe explains. “It’s a lot like how tooth implants work, actually.”
So, bottom line: Will Eisen be able to golf again?
Dr. Wolfe is optimistic: “Right now it’s a lot of theory. We’ve tested it; it took all kinds of experiments to show that it actually does work, and that people do get that dart throwing motion using this wrist implant. But we’ve done all of two so far.” Eisen’s was the first; another patient in Florida received the new wrist implant just last week.
Still, things are looking good: the first-generation design, the hemiarthroplasty, has been successfully implanted in many UK patients.
“We’ve done 25 or 30 of them and they’re holding up beautifully,” says Dr. Wolfe. “We have golfers golfing, and all sorts of things. So we have every reason to believe this will be an important contribution to science and to clinical practice.”





